Around 70 people took part in our conference (a limited number participated ‘online’ via ‘online streaming’). Participants came from Belgium, Canada, Germany, England, Georgia, the Netherlands, Austria and Sweden.
During our conference we also celebrated our 25th anniversary.
We received, among other things, congratulations via a video message from Prof. Dr. Jan Peter Balkenende (Former Prime Minister, External Senior Advisor to EY, Professor Erasmus University, Ass. Partner Hague Corporate Affairs.), Dr. Yann le Camm (CEO Eurordis) and Pamela Gavin (Executive Vice President NORD – USA).
Finance and other discussed items
As chairman of the CMTC-OVM organisation, Lex opened the conference. The minutes of the previous member conference were approved. Subsequently, the financial data and the positive findings of the Audit Committee were presented, after which those present discharged the board treasurer for the 2020 financial year.
The minimum membership fee for the year 2021 is the same as in 2020 and is 35 euros.
The budget for the year 2022 was presented, whereby it should be noted that we have submitted a subsidy application for this to the Ministry of Health, Welfare and Sport (VWS) which is still being processed.
The following points were discussed:
- The Complaints Committee has not received any complaints.
- The CMTC-OVM organization: we would like to expand the board with two new functions, namely: ‘youth representative’ and ‘patient advocate coordinator’. We are still looking for candidates for this.
- Overview of the main activities carried out in 2020. An impressive list!
- Planned activities for 2023 where we assume that the pandemic will subside considerably so that (international) meetings can be organized again.
- Budget 2023.
- Our planned, in progress and completed projects. Important is our global Patient Advocates project: Patient Advocates from all over the world come to the Netherlands at our expense for training and to attend our global conference at the end of October 2022.
- Personal stories. These are widely read. It would be nice if more people would like to share their personal story.
Presentation Dr. Alyson Norman (United Kingdom)
Living with a visibly different appearance
In her lecture, Dr Alyson Norman discussed the psychosocial impact of appearance-related distress. She also introduced the FaceIT@home tool an online web tool for adults to learn to cope with visible difference.
FaceIT@home consists of a web-based interface with 7 main sessions and a follow-up session for users 12 weeks after the main course.
A large number of individuals experience appearance-related distress (around 30% of those with visible difference) and therefore there is a need for support in this area. However, there are many barriers for these people, such as geographical barriers, disabilities and stigma The web tool addresses these barriers by allowing individuals to use the tool in their own homes without having to be supported by a health professional. However, the tool is also flexible enough to be used alongside standard psychological therapy, can be used by individuals waiting for other services or can be used as a ’top-up’ after therapy has ended. Within the presentation, Norman discusses how Face IT can be used at lots of different levels of intervention, from a basic resource information tool through to a stand-alone psychological therapy or facilitated by a therapist or health professional.
If anyone is interested in using the tool: contact Norman via email: alyson.norman@plymouth.ac.uk
A lived experience group is being developed to help make future changes to the tool and they would welcome any individuals with a visible difference or family members to get in touch if they would like to be part of this group. A young person’s version is also available that is aimed at individuals who are aged 12-17 years.
Presentation Dr. Kakha Bregvadze (Georgia)
Raising awareness about rare diseases in Georgia
Dr Kakha Bregvadze talked about what he and his colleagues are doing to raise awareness about rare diseases in his country and enable and improve diagnosis and treatment options.
Globally, rare conditions affect between 3.5% and 5.9% of the population meaning that anywhere between 263 million and 446 million people are living with these in the world. Approximately 80% of rare conditions are of genetic origin. Despite its prevalence, the landscape of rare conditions is often plagued with challenges across the patient journey.
Georgia
Georgia is a small country with a population of 3.7 million and awareness of rare conditions is still low among patients, physicians, and members of the general public. “Our team’s goal was to raise awareness in the country and enable/improve diagnosis and management options”, says Bregvadze. “In 2018-2020, we took part in the biomarker clinical trial with Centogene, a German-based biotech company. Before enrolment in the trial, patients were offered genetic testing for free. As a result, almost 3000 individuals received genetic testing over a 4-years period and many patients finally got the diagnosis. Interestingly, WES (whole exome sequencing) had a diagnostic yield of up to 60% in a cohort of clinically well-characterized patients with neurodevelopmental disorders, the majority of which were caused by novel de novo mutations.”
Collaboration
The team of Bregvadze also collaborated with Face2Gene (https://www.face2gene.com/) to conduct several workshops on the application of artificial intelligence in the diagnosis of rare conditions for healthcare professionals and medical students. Furthermore they established a close collaboration with McGill University (Montreal, Canada)on the disorders of peroxisomal biogenesis (Peroxisome biogenesis disorders (PBD) are a group of conditions caused by a partial or generalized defect in peroxisome biogenesis). Other collaborations include: the University of Bonn on the application of artificial intelligence in clinical practice, Helse Bergen university (Norway) on rare diseases, and with King Faisal Specialist Hospital (Riyadh, Saudi Arabia) on rare and undiagnosed disorders for identification of new disease-causing genes, as well as with European Joint Programme on Rare Diseases (EJPRD), Undiagnosed Diseases Network International (UDNI), and the European Society of Human Genetics (ESHG).
Activities to raise awareness of rare diseases
Bregvadze: “We have initiated the ‘Rare conditions’ section in one of the largest Georgian medical social media groups ‘MedCity’, where information about a specific rare condition is uploaded in the Georgian language on a weekly basis. We visited multiple TV/Radio shows and closely collaborated with patient advocacy groups. These collaborations resulted in establishing governmental programs providing care and the treatment for patients. We cooperated with CMTC-OVM, Unique (Understanding Rare Chromosome and Gene Disorders, UK), and many other organizations and translated various guides for patients/healthcare professionals into the Georgian language. A Georgian Society of Medical Genetics and Epigenetics was founded. Many new patient organizations were established. Based on these activities, awareness of rare conditions among health professionals and the general public began to increase. Our goal for the future is to promote the education of healthcare professionals and students to recognize rare conditions, support the formation of patient advocacy groups, negotiate with the government to support patients with rare conditions, and facilitate the improvement and expansion of the national NBS program.”
Presentation Prof. Dr. Miikka Vikkula
The genetic cause of vascular malformations (update 2022)

Thirty years ago, there was absolutely no knowledge about the cause of the development of vascular malformations (VMs). Until at some point researchers started investigating VMs that occurred in certain families. The idea was that if it occurs in certain families then there must be a genetic cause.
This research led to the discovery of 13 different types of VMs that are heritable (the first discovery was in 1994). The genes containing the mutations that cause these malformations have been identified.
Most mutations that occur in these genes are loss-of-function mutations that is, the product of the gene, the protein, does not work at all or works less well. The mutation in the TIE2 gene is an exception: it results in a ‘gain-of-function’, the protein works too well.
‘Second hit mutation’
One of the remaining questions was: why do the lesions occur only in certain areas of the body? That was solved by the discovery (2002) of a second mutation. Normal cells have two copies of each gene, one from the father and one from the mother. In the hereditary variant of VM, one of the two copies already has a mutation at birth. Later in life, a second mutation (somatic mutation) then occurs in the other copy of the gene. If both copies of a gene have the pathogenic mutation, this leads to the disease. In the tissue where the second mutation occurs, the clinical signs occur. Multiple second hit mutations have now been discovered for most earlier inherited mutations.
In sporadic vascular malformations (non-hereditary form), researchers looked for somatic mutations that could be responsible for the malformation. Since 2009, many somatic mutations associated with certain VMs have been found, as for example PROTEUS is associated with a somatic activating mutation in the AKT1 gene.
Latest findings
SWS
Sturge Weber Syndrome (SWS) is often associated with a mutation in the GNAQ gene. Recently, three SWS patients have been studied who have a GNA11 mutation. They have slightly different features than most GNAQ-SWS patients. Radiologists need specific MRI to detect this form of SWS.
CMTC
Although a mutation in the GNA11 gene is associated with CMTC in some cases, it is not the case in all patients. It is not known whether this is due to the fact that the mutation is technically difficult to detect because it is very little present or whether it is a mutation in another gene.
Laboratory animals
Laboratory animals (pre-clinical models) are indispensable for doing research on VMs. If you introduce the same mutations found in VM patients into mice, they develop the same lesions as the patients. These mice can be used for testing drugs (inhibitors) to investigate if the lesions reduce. For example, rapamycin was tested in a mouse model with a TIE mutation; the growth of lesions stopped.
You can also investigate in which organs more lesions occur. In a KRAS (mutant) model, besides the brain, there were lesions in the intestine, liver and lungs. Trametinib reduced the lesions in this model.
AVMs
Thalidomide proves very effective in patients with severe arteriovenous malformations (AVMs).
Increasingly, therefore, drugs can have a beneficial effect on the course of VMs.
Presentation Prof. Dr. Laurence Boon

Vascular malformations/anomalies can occur anywhere in the body and in different tissues. Hence, patients with vascular malformations (VMs) are best discussed in a multidisciplinary team for proper diagnosis and treatment as is done at the hospital where Professor Laurence Boon works, Saint-Luc University Hospital in Brussels.
In her lecture, Boon discussed the different types of malformations (capillary, lymphatic, venous and arteriovenous malformations) and discusses the forms of treatment used so far such as surgery, laser, sclerotherapy and medication. Below is a brief overview of medication.
Sirolimus
In a phase IIa clinical trial, Boon’s team treated patients with slow flow malformations (VMs) (PIK3CA or a TIE2 mutation) with sirolimus. Coagulation went down, pain was reduced and quality of life was much improved. This was followed by a phase IIb prospective clinical trial (more patients than in IIa, n=19), in which the efficacy of sirolimus was confirmed. Now a phase 3 clinical trial (250 patients) is under way (several research groups are participating in this) to get the many remaining questions answered. It is especially important to find out which treatment is best for which type of malformation.
It is now known from the trial that sirolimus can suppress pain. It also stops bleeding and stops/reduces oozing. Functional limitations may improve such as vision or voice if the malformation is located there. It can also reduce the size of a VM or LM.
Sirolimus also has side effects including asthenia (weakness), mucositis (inflammation of the mouth-gastrointestinal mucosa), diarrhea but these are often well managed. About 15% had serious side effects.
Conclusion: sirolimus is effective for relieving symptoms and useful before embarking on interventions such as surgery. It has become the gold standard for medical treatment of slow flow VMs; however, it is not yet approved by the FDA/EMA.
Alpelisib
Alpelisib (PIK3CA inhibitor) is approved in the US for the treatment of PROS (PIK3CA-related overgrowth syndrome). With this, good results (size reduction) have been obtained in aggressive forms of PROS. Also reduction of adipose tissue is obtained. But it is a more complicated treatment (type 2 diabetes may occur after treatment with alpelisib) and the long-term effects are not known.
Miransertib
PROTEUS treatment with miransertib (AKT1-inhibitor).
Thalidomide and trametinib in AVM
Sirolimus does not work well in arteriovenous malformations (AVM). Thalidomide does work well in AVMs, especially pain went down tremendously and bleeding stopped. Trametinib also works well but annoying side effects such as severe acne.
Presentation Prof. Dr. Chantal van der Horst
Pain and Appearance in patients with Vascular Malformations

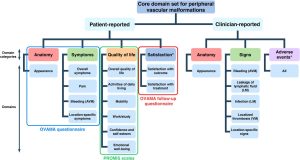
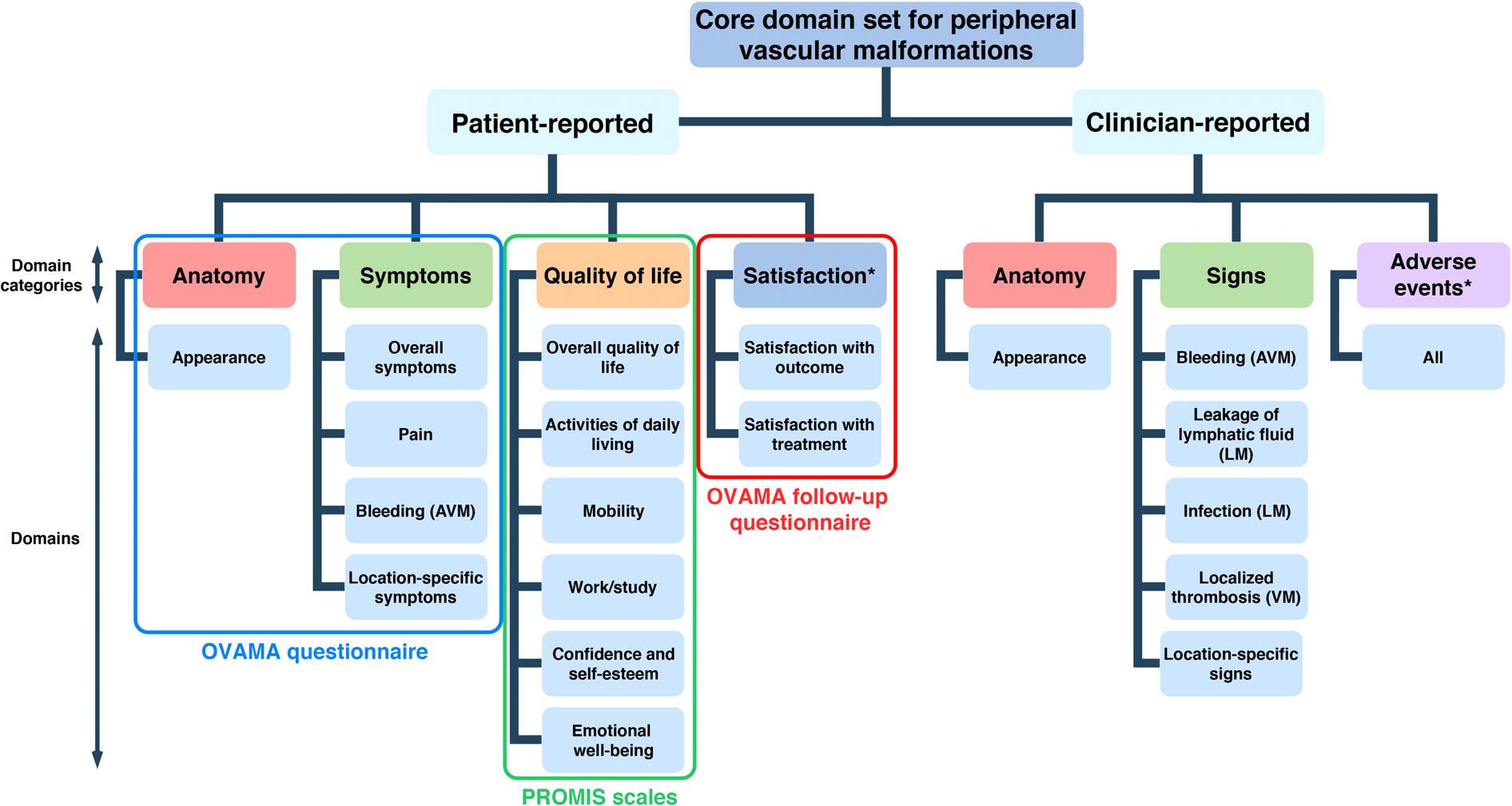
OVAMA-questionnaire
The problems that matter most to patients with vascular malformations can be evaluated from the patient’s perspective by using the OVAMA questionnaire (https://ovama.org/ovama-questionnaire/ ) which is developed with the participation of patients and professionals all over the world (including ISSVA). Treatments can be evaluated and compared for effects on these core outcome domains (see figure. The many applications of the OVAMA questionnaire may significantly improve research and, ultimately, the care for patients with vascular malformations.
Van der Horst: “We asked patients treated in our center to fill in the OVAMA questionnaires(Q) and also Q on quality of life. Filling in these ‘Q’ is quite a task for patients and parents of patients although we have tried to make the process of filling in as easy as possible. Until now this is the only and very important way to have adequate information on how patients experience having a vascular malformation.”
Two studies
“We performed two studies:
- Appearance-related concerns and their impact on health related quality of life (HR-QoL) in patients with peripheral vascular malformations.Conclusion: severe appearance-related concerns were present in 2/3 of patients with VMs, impairing their mental HR-QoL. Clinicians should acknowledge appearance-related aspects, monitor psychological well-being, and offer intervention aimed at improving satisfaction with appearance.
- Clinical characteristics associated with pain in patients with peripheral vascular malformations.
Conclusion: pain is a frequently reported complaint in patients with VMs and is present in approximately one-half of patients. Patients with lesions located in the arms or legs, lesions in muscle or bone, and female patients are more likely to experience pain. The presence of pain negatively impacted patients’ QoL and our study shows that pain is a serious concern and needs to be actively assessed. Pain is a sign of various etiologies and should be examined to properly treat the pain.”
Prof dr Chantal van der Horst Plastic surgeon; collaborator Centre of Vascular Anomalies Amsterdam UMC, head: Dr. N. van Hout.
Author list: Merel L.E. Stor, M.D.a, Max M. Lokhorst, M.D., Ph.D.a , Sophie E.R. Horbach, M.D., Ph.D.a, Danny A. Young-Afat, M.D., Ph.D.a, Phyllis I. Spuls, M.D., Ph.D.b,c, Chantal M.A.M. van der Horst, M.D., Ph.D
Workshop by Johannes Verheijden (the Netherlands)

Particularly nice to see that participants are extremely involved and feel safe and dare to show openness to share their experiences. Nevertheless, it would be advisable to give the workshop twice: once in Dutch (most of the participants were Dutch) and once in English, so that all parties can participate optimally and language is not a barrier to active participation.
Workshop Dr. Margaret Lee (USA)
Comfortable In Our Skin: Strategies for Confidence & Success

Presentation Dr. Marije van Dalen (the Netherlands)
A visible condition (e.g. a cleft lip, wine stain or eczema) in the face or on the body occurs in 1 in 44 people. It is estimated that one-third of this group experiences negative psychological consequences.
This presentation describes research on Face IT for young people, an online eHealth program for young people (12-18 years) with a visible condition that promotes psychological well-being. Face IT for young people consists of eight sessions of half an hour. In these sessions, young people learn to deal with difficult social situations and learn to change difficult thoughts into more positive thoughts. They learn techniques through social skills training and cognitive behavioral therapy. The program can be followed at home.
Young people who have followed Face IT for young people appreciate the program and would recommend it to other young people with a visible disorder and appearance-related stress. An international study together with Norway shows that young people who have followed Face IT for young people report less social anxiety than young people who have not followed the program.
In addition, the psychological well-being of children and young people with a visible disorder and their parents were investigated. Children with a visible disorder under the age of 12 show fewer behavioral and emotional problems than their peers without a visible disorder. However, young people aged 12 to 18 with a visible disorder experience more anxiety symptoms than their peers.
Research on parents of children under the age of 12 with a visible disorder shows that they report less stress and better psychological well-being than other parents.
Workshop Nienke Oosting & Eva Vroonland (the Netherlands)

This information contains the wishes and needs that the visitors have with regard to the organisation. The board would like to know this, in order to get the best possible picture of which activities best meet the needs of the members. This in order to really make a difference and to support you as best as possible.
Eva Vroonland and Nienke Oosting discussed the various workshops of the day with the visitors, based on the following three questions:
- What of the CMTC-OVM offer do you find important?
- Suppose you can help determine which activities and/or policy will be on the agenda. Which activities and/or policy would you put high on the agenda?
- Which parts are receiving too much attention? In other words, what should be given less priority?
In addition, Eva and Nienke discussed these questions with the participants in a workshop of 45 minutes. Three board members of CMTC-OVM discussed a question with different groups. Eva and Nienke were enthusiastic about the openness with which visitors entered into a conversation with them and the board members. New insights have been collected, which the board will work with, together with you.
Video presentations (members only)